Hospital trusts fear the removal of mass free Covid testing is “premature” and likely to exacerbate health inequalities, a leading NHS chief has warned, as infection levels in England reach new highs for the pandemic.
Samuel Lovett www.independent.co.uk
Chris Hopson, the chief executive of NHS Providers, which represents all trusts in England, said there was “nervousness” in the sector at the “speed and scale” in which free testing has been scaled back, adding that members “would have preferred” to keep the policy in place “until we were further through this”.
The move comes at a time of record-breaking infection levels: one in 13 people in England caught the virus last week, according to the Office for National Statistics (ONS). This amounts to 4.1 million infected individuals.
Hospital admissions have also risen in recent weeks, showing that the NHS still faces “significant risk” from the virus, Mr Hopson told The Independent.
Under current guidance, free testing will continue to be provided for hospital patients and patient-facing staff, those who remain vulnerable to Covid-19 and are eligible for community drug treatments, care home residents and people working in some high-risk settings, including prisons.
Along with numerous campaign groups and scientists, NHS trusts are particularly concerned by the prospect of poorer communities bearing an even greater burden of disease due to the inability to afford regular testing.
“One of the issues is inequality, where we are now in a position in which people are potentially able to look after their health better if they’re able to afford tests, compared to those who can’t,” said Mr Hopson.
“That feels deeply uncomfortable given that the NHS is based on the fundamental principle of care being available for free at the point of use, based on clinical need, not ability to pay. This impact on health inequalities is the concern I hear most from our members.”
The most deprived parts of England have been hardest hit throughout the pandemic, while recent analysis from The Independent showed that at least 30 per cent more coronavirus deaths occurred in these areas in the first six weeks of the year.
Separate ONS data also shows that poorer regions in the country are a greater risk of re-infection, with the now-dominant Omicron sub-variant, known as BA.2, known to be capable of repeatedly infecting people over a matter of months.
Although Mr Hopson acknowledged the government has “difficult decisions” to make in managing the “trade-offs between costs and public health protection,” he warned that the details of the new testing regime for hospitals could have an adverse impact on operations.
Previously, patients penned in for surgery were required to carry out a PCR test in the days before their appointment. “We knew where people stood before they came to the hospital,” Mr Hopson.
Now, patients are required to return a negative result via a lateral flow test “in advance of admission,” NHS guidance states.
“There’s a nervousness that in switching to on-the-day LFT testing, as opposed to advanced PCR testing, where trusts have been providing results before patients travel in, we’ll see more people coming in and saying ‘I didn’t realise I was meant to have an LFT test’,” Mr Hopson said.
“That could mean greater levels of cancellations on the day, just at the point when we are trying to maximise elective operation throughput.
“Trust leaders are nervous about the impact of making what might seem to be small changes, when actually they could have quite a significant operational impact. We’ll need to work through the details of exactly what this new regime means.”
Fears are also mounting over the persistence of hospital-acquired infections (HAIs) as BA.2 continues to spread throughout the UK. In the past 28 days, 23.7 per cent of people in hospital with Covid caught the virus after being admitted for a separate health issue, data show.
Although free testing will continue to be available for patients and their doctors and nurses, ancillary staff and visitors are not eligible. This risks repeatedly exposing already sick patients to the virus, said Mr Hopson.
“Another area of nervousness is protecting the much larger number of vulnerable and immunosuppressed patients we see in healthcare settings,” he said.
With BA.2 bringing the issue of HAIs back into focus, there is concern that the new testing policy regime could endanger trusts’ most vulnerable patients, Mr Hopson suggested. “Are we striking the right balance here between, again, the public cost of testing versus ensuring we’re doing everything we can to protect people?”
Added to the threat posed by on-ward infections, the number of people admitted to hospital, both with and for Covid-19, rose last month, while prevalence levels in the community are currently at record highs.
There were 15,632 people in hospital in England with Covid as of Wednesday, up 18 per cent week on week, and the highest figure since 19 January.
While roughly half of patients in hospital with Covid were receiving treatment for other health issues, numbers are also rising in primary Covid hospitalisations, while admissions in over-65s are now 15 per cent higher than their January 2022 peak.
“As we can see from current levels of hospitalisations, which have gone up over the last few weeks, we still face significant risk in terms of Covid being around and I think there’s nervousness about we simply don’t know what and how this virus is going to develop,” he said.
Given the current context, trust leaders “would have preferred to have had availability of free testing for a longer period until we were further through this and we were in more of an endemic state,” Mr Hopson added.
“People are nervous this is premature and what they’re particularly nervous about are the health inequality consequences and the impact on vulnerable patients.”
Professor Tim Spector from King’s College London, who runs the Zoe Covid tracking app, told Times Radio the timing for the end of free testing “couldn’t really be worse”.
The latest estimates from the ONS show that 4.9 million people in the UK were infected with Covid-19 between 20 and 26 March, up from 4.3 million in the previous week.
Kara Steel, senior statistician for the ONS Covid-19 infection survey, said: “Infection levels remain high, with the highest levels recorded in our survey seen in England and Wales and notable increases among older age groups.”
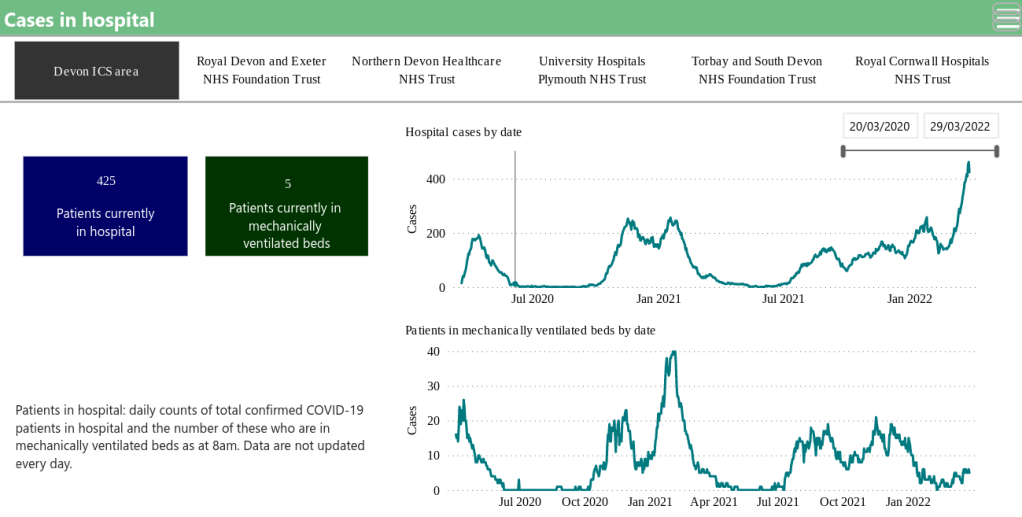
Latest Hospital data for the Devon ICS (includes all hospitals in the County)